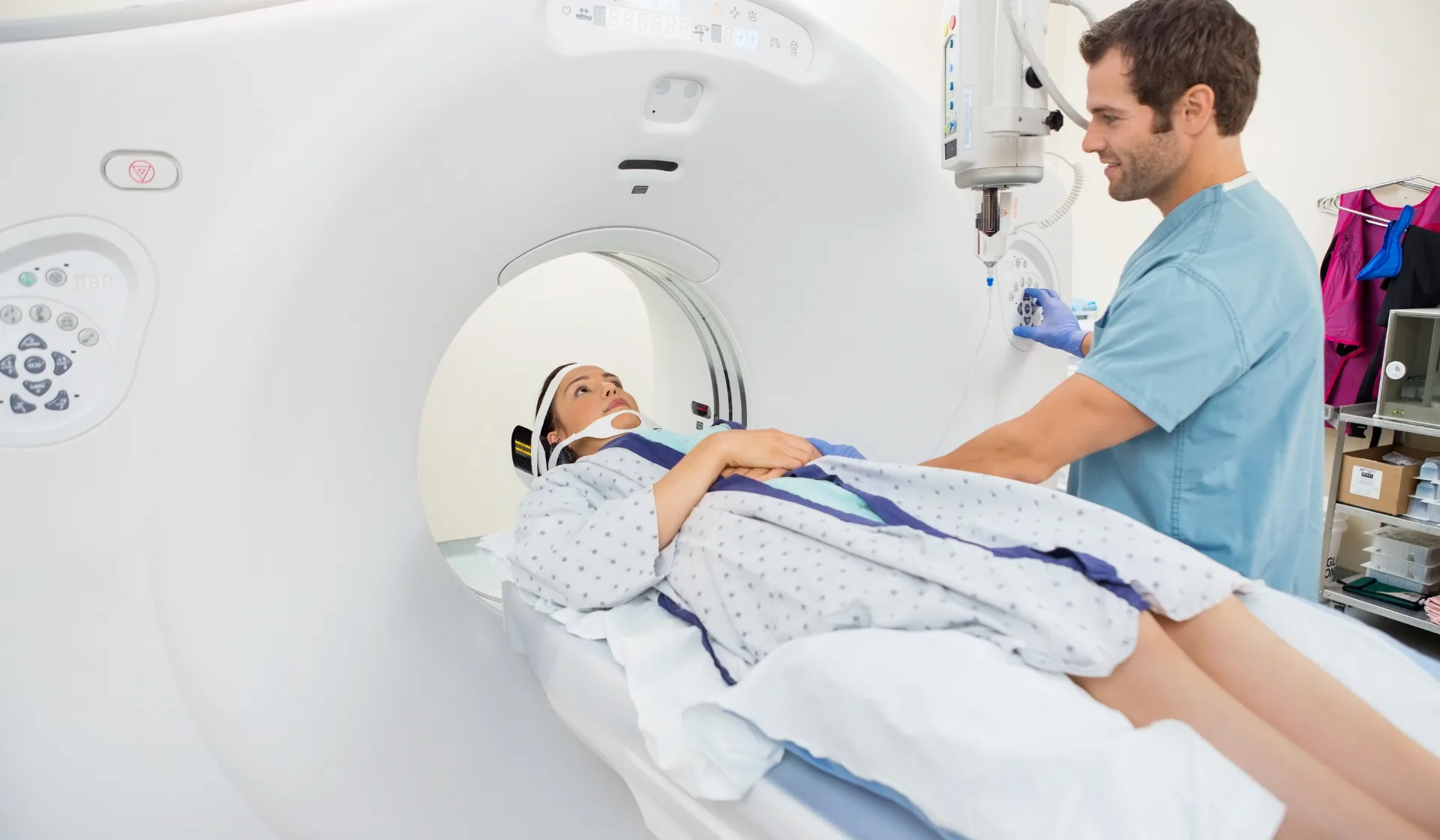
People in pain used to, at first, feel reassured by getting a scan. Then often the pain would stay for weeks or months. Drugs would be thrown at it and if that didn’t work surgery seemed like the next logical step. It seems to make sense that the answer would be hiding somewhere in the soft tissue like a tear, a bulging or slipped disc, etc. But chronic pain or pain that doesn’t have a clear causation is elusive to high tech scans and images. In many cases the more valuable next step is not another kind of picture inside your body, or a diagnosis, or a masking medicine, but a thoughtful practitioner who is guided by science and who understands how pain actually works.
That distinction matters because pain is usually not a sign of tissue damage, even if the pain is unbearable. Modern pain science has moved beyond thinking that tissue injury is necessary for pain. Pain is increasingly understood as a sensitivity in your nervous system and an interpretation by your brain of something happening in your body, shaped not only by a tissue issue but more often a result of a threat, a prior past experience, stress, fear, beliefs, and broader biopsychosocial context.
This does not mean pain is imaginary. Pain is real, and reality is more complex than physical or structural problems alone. When pain is persistent and has lasted over time, the nervous system can become highly sensitive and reactive, even when the original tissue issue has healed or is no longer the main driver.
This is why scans can be both useful and limited, they only show physical changes, and for decades we’ve been interpreting those changes wrong. With the massive amounts of data we have today we initially presume the limitations of technology and the alternative and less invasive therapies have become the go to response to pain. Imaging has an important role when a clinician suspects serious pathology, specific structural injury, or a condition where the findings would meaningfully change management. But outside those contexts, especially in many persistent musculoskeletal presentations where there isn’t a clear causation, imaging often adds far less clarity than people expect and any misinterpreted structural anomalies often increase fear and anxiety which in turn increase pain. An example that has been very well documented in the research as a classical misinterpretation of a torn spinal disc is that, just as we age after 25 years old and begin to have wrinkles, what were interpreted as tears are now more precisely known as internal wrinkles. Believe it or not.
Research on chronic pain neuroimaging reflects this tension. Neuroimaging has helped researchers understand that persistent pain is mulit-dimensional and is not reducible to only a single physical problem. At the same time, major reviews caution that neuro images should not be a standalone answer to a person’s pain, but should be used as one tool, and certainly not a replacement for the patient’s lived report or a skilled assessment. Research is now recommending against early scanning.
Standard structural scans can mislead when they are interpreted without life context. Findings such as degeneration, disc bulges, and other anatomical changes may sound alarming, yet many reports of structural discrepancies are common in people without pain. That means a scan can sometimes intensify fear, reinforce a fragile story about the body, and inadvertently increase the sense of threat that keeps pain active. Simply put, keep moving. The question becomes, How?
This is where the right practitioner becomes more valuable than scans and diagnoses. A thoughtful practitioner does not dismiss symptoms, but sees them as part of a bigger story. Good practitioners don’t over react to every sensation that correlates with positive (or negative) imaging results. They know how to screen for red flags, identify when imaging is truly necessary, and recognize when the clinical picture points more toward a sensitized or overprotective nervous system than a dangerous structural problem.
Just as important, they know how to explain pain in a way that changes the experience of it. Pain neuroscience education has become a meaningful part of care for persistent musculoskeletal pain because it helps people reconceptualize pain as less threatening and guides us to more modern and thorough approaches to change. Reviews of the literature suggest that understanding the neuroscience behind pain can reduce pain, disability, catastrophizing, fear of movement, and psychological distress, especially when it is paired with hands-on therapy, movement coaching, and exercise. Neuroscience encourages sincere practitioners to think outside the box and treat the person not only the symptom.
That combination has become central to modern pain treatment. Surgery is often premature, drugs need to be used conservatively and down the line in treatment, and education alone is not a magic trick either. Movement alone can fail when the person remains trapped in a story of damage and danger, or because their compensations have lead to “movement amnesia.” But when a patient begins to understand that pain is not always an accurate measure of tissue health, the body often becomes a place they can work with again instead of a place they must constantly fear.
A practitioner grounded in neuroscience listens for various factors that a scan cannot capture. Things like sleep patterns, nervous system load, repeated guarding, fear of reinjury, hypervigilance, life stress, previous injuries/surgeries, and the subtle ways a person has adapted to pain. Those details are not side issues. In persistent pain, they are often part of the main mechanism keeping the problem alive.
This perspective is not anti-imaging. It is anti-simplicity. It respects the value of scans while refusing to mistake a tool that focuses on one aspect rather than the whole truth. The goal is not to prove that structure never matters. The goal is to avoid collapsing a deeply human, nervous-system-mediated experience into a single image and then acting as though the image is the whole.
The deeper clinical question is not only, “What does the scan show?” but also, “What is this person’s nervous system protecting them from, and why has the volume remained so loud?” That question opens the door to better and more creative assessments, better treatment options: clearer education, more relevant solutions, a plan for graded exposure to movement, exercise criteria, calmer interpretation of symptoms, and a therapeutic relationship between client and practitioner that restores confidence rather than amplifying fear.
In many cases, that is the turning point. Not a new image, but a new understanding. Not another search for what’s damaged, but a more skillful reading of pain itself and a more precise plan to get out of it.